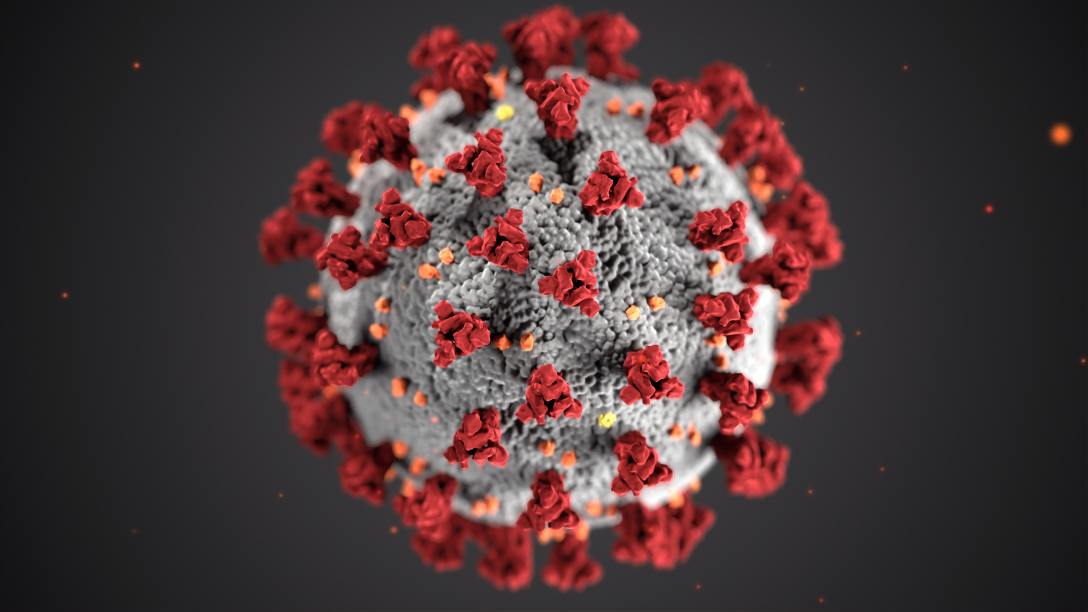
Well, I suppose it’s time to address the elephant in the room. Or in this case, the virus we’re hoping to keep out of the room, COVID-19. Most people know it as coronavirus, but to only call it coronavirus is technically incorrect. COVID-19, the virus that is currently taking the world by storm, is actually just a new strain, or type, of coronavirus. To further clarify: It is NOT a type of flu or cold virus. It is a new strain of a structurally different type of virus, coronavirus. Signs and symptoms of COVID-19 most commonly include a fever, dry cough, tiredness, and difficulty breathing in severe cases. It is a virus that attacks the respiratory tract.
Unfortunately, over the past few weeks the spread of COVID-19 has officially become a pandemic. At the time I’m writing this, there have been 294,110 confirmed cases and 12,944 deaths from COVID-19 across 186 countries, areas, or territories. Out of these numbers, 15,219 confirmed cases and 201 deaths were in the United States alone. However, these numbers will likely continue to greatly increase over the next few weeks, as more people will begin to show symptoms and the amount of testing is increasing. So far China has been hit the worst, with 81,499 confirmed cases and 3,264 deaths. Italy also has the largest death rate from the virus, as they have had 53,578 confirmed cases and 4,827 deaths. This is likely because Italy has a high population of elderly adults who will have a harder time fighting off a virus their body has no antibodies for. Again, these numbers are likely to fluctuate over time, but they give the most accurate picture of what is happening at the time I am writing this blog. If you are interested in the numbers, be sure to follow the CDC or WHO for their official reports.
Now you may be wondering, or you may know someone else that is wondering, why is the world so worried about this? Why are we shutting things down and encouraging quarantine? Why should I be worried about it if I’m young and have a good immune system? Well, the reason why everyone is worried about the virus is because there is something to worry about. While it isn’t something worth going absolutely nuts about (looking at you, toilet paper hoarders), it is something we need to do our best to contain and prevent the spread of. The reason we are most worried about the virus is because of its long incubation period. This means that, unlike when we contract something like the flu and know within the first day or two we have come into contact with the virus, we can be infected with COVID-19 for anytime up to two weeks before we begin to feel the effects and know we are infected. This means that we can be infected for up to two weeks and unknowingly spreading the virus to anyone we come in contact with or anyone who touches the same things we touch. While this might not mean anything to us, it can mean the world, and even life or death, to others who we come into contact with during this period, or to someone who comes into contact with the person we came into contact with. For example, if you were walking around unknowingly infected, coughed or sneezed near a man, but then that man went home to take care of his elderly parents or immunocompromised child, you could have played a part in spreading a virus that some people’s bodies cannot fight off. Point blank, your spring break trip or night out at the bars is not worth the potential of someone else down the line becoming infected and dying. Additionally, because this strain of virus is new, no one has antibodies to it. When anyone becomes infected with it, it will likely be very uncomfortable and tiring, as our bodies have to work even harder than normal to rid ourselves of the infection. It is for THESE reasons, not unfounded panic or anything like that that the CDC, WHO, etc., have all suggested social distancing. It is also because of these reasons that many other changes are being made in areas affected by the virus, such as universities transitioning to online classes, bars and restaurants being closed, gatherings of more than 50 people being banned, etc.. Social distancing and self quarantine are some of the most important things we can do to slow down the spread of the virus so that it doesn’t go beyond what our healthcare infrastructure can handle. This means that less people are infected or dying, and more people will get the healthcare they need if they are a severe case or immunocompromised.
While I’m sure this blog hasn’t answered every question you may have, I hope it has at least explained some things and given answers to some questions. I hope that, in the very least, you have learned what COVID-19 is, how it has become a pandemic, and why social distancing and self quarantine is important. While at a time like this, with so many things happening and so many uncertainties, please do not panic. The best thing you can do is relax, spend as much time at home as possible, and limit your contact with others. Be sure to wash your hands frequently and avoid touching your face. Instead of going out, watch some movies, donate to charity or other people in financial need, spend time with your immediate family that lives with you, and do your part to prevent the exponential spread of the virus and preventable deaths. If you have any more questions, please consider viewing the websites of the CDC or WHO for more information.
Featured photo by Kelly Sikkema on Unsplash.